
Has your doctor suggested anesthesia for endoscopy, or are you considering requesting it yourself? Here’s a clear guide to help you understand the process and what to expect.
(Estimated time of reading: 2min)
Counseling and Preparation
Before your procedure, you won’t be able to consume:
- fried, fatty foods, or meat for 8 hours.
- light meals or non-human milk for 6 hours.
- water for 2 hours [1].
Additionally, if undergoing a colonoscopy, you must follow a strict diet on the days before your exam to ensure a clear examination field (bowel preparation).
Anesthesia Screening
An anesthesiologist evaluates your medical history to design a tailored anesthesia plan. This crucial assessment minimizes risks and usually occurs on the procedure day.
Type of Anesthesia and Consent
Light to moderate sedation is the most frequent type of anesthesia for endoscopy [2,3]. The choice depends on your health and the procedure’s complexity [2]. Thereafter, you review and sign consent forms outlining benefits and risks.
The Procedure
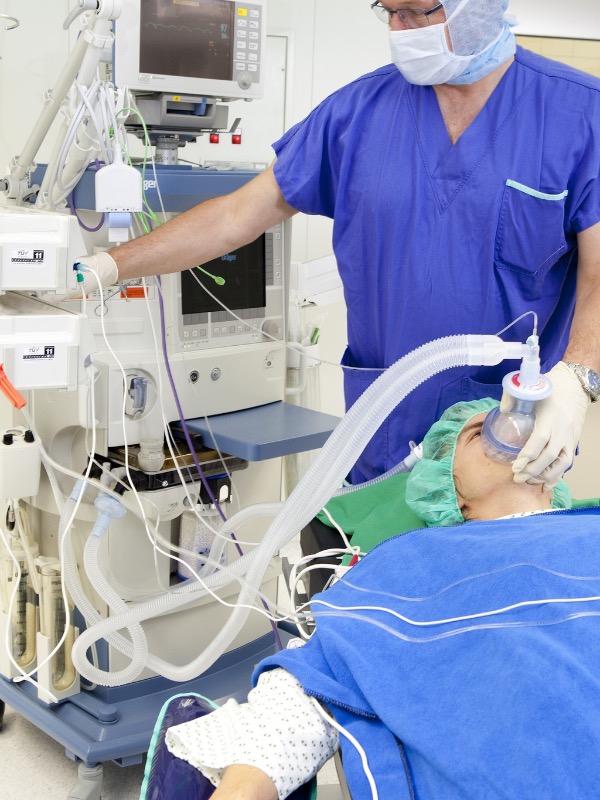
Vital signs are closely monitored, and oxygen is provided via a cannula or mask, while intravenous sedatives (e.g., benzodiazepines, opioids, propofol, etc.) are administered. Sedation levels vary:
- Light Sedation: you remain calm but aware, with potential memory gaps.
- Moderate Sedation: you’re drowsy and likely won’t recall the procedure.
- Deep Sedation/General Anesthesia: you’re fully unconscious [4].
Post-Anesthesia Care
Recovery is typically quick, and most patients go home the same day [2]. Arrange transport home as you won’t be able to drive and avoid making critical decisions for 24 hours.
Conclusion
Anesthesia for endoscopy is a safe, well-managed procedure tailored to individual needs. Proper preparation, evaluation, and care ensure optimal outcomes and a smooth recovery. Talk to your healthcare team for personalized advice and reassurance.
P.S.: Less stressed about your endoscopic examination? Leave a comment below. Let’s talk about health! Also, if you’d like to uncover more of anesthesia’s secrets, please check my previous blog post here.
References
[1] Practice Guidelines for Preoperative Fasting and the Use of Pharmacologic Agents to Reduce the Risk of Pulmonary Aspiration: Application to Healthy Patients Undergoing Elective Procedures: An Updated Report by the American Society of Anesthesiologists Task Force on Preoperative Fasting and the Use of Pharmacologic Agents to Reduce the Risk of Pulmonary Aspiration. Anesthesiology. 2017;126(3):376-393. doi:10.1097/ALN.0000000000001452
[2] Sharp CD, Tayler E, Ginsberg GG. Anesthesia for Routine and Advanced Upper Gastrointestinal Endoscopic Procedures. Anesthesiol Clin. 2017;35(4):669-677. doi:10.1016/j.anclin.2017.08.006
[3] ASGE Standards of Practice Committee, Early DS, Lightdale JR, et al. Guidelines for sedation and anesthesia in GI endoscopy. Gastrointest Endosc. 2018;87(2):327-337. doi:10.1016/j.gie.2017.07.018
[4] Statement on Continuum of Depth of Sedation: Definition of General Anesthesia and Levels of Sedation/Analgesia. https://www.asahq.org/standards-and-practice-parameters/statement-on-continuum-of-depth-of-sedation-definition-of-general-anesthesia-and-levels-of-sedation-analgesia
Leave a Reply